2 results
Optimizing COVID-19 Symptom Screening in the Pediatric Population
- Geena Zhou, Prachi Singh, Emily R. Perito, Naomi Bardach, Nicole Penwill, William Burrough, Ann Cheung, Margaret Nguyen, Shalini Mittal, Grace Cheng, Mia-Ashley Spad
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s55-s56
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Research analyzing COVID-19 symptom screening has primarily focused on adult patients. In efforts to safely reopen schools, symptom screeners are being widely utilized. However, pediatric-specific outpatient data on which symptom combinations best identify children with COVID-19 are lacking. Such data could refine school symptom screening by improving screener sensitivity and specificity. In this study, we assessed the frequency of symptoms and symptom combinations in children tested for SARS-CoV-2 in outpatient settings. We aim to contribute to the optimization of pediatric COVID-19 screening questionnaires, to ultimately minimize both COVID-19 transmission in schools and missed school days. Methods: We conducted a retrospective analysis of outpatient symptoms screens, SARS-CoV-2 test results, and demographics of children (≤18 years) tested for SARS-CoV-2 between March 30 and November 30, 2020, at 3 UCSF-affiliated COVID-19 outpatient screening clinics in northern California. Those with incomplete symptom screens, >7 days between symptom documentation and test, and invalid test results were excluded. Results: Of 473 children tested at 1 site, 21 children had positive SARs-CoV-2 results and 452 children had negative results (4.4% positivity rate). Moreover, 85.7% of SARS-CoV-2–positive children had a known exposure to COVID-19 (Table 1). Of SARS-CoV-2–positive children, 61.9% had >1 symptom. Also, 52.4% of SARS-CoV-2–positive children had at least 1 symptom (fever, cough, or loss of taste or smell) versus 62.8% of SARS-CoV-2–negative children (Table 2). Runny nose or nasal congestion was the most frequently reported symptom in the SARS-CoV-2–positive group (47.6%) as well as the SARS-CoV-2–negative group (58.6%). Also, 14.3% of SARS-CoV-2–positive children had eye redness or discharge versus 3.1% of SARS-CoV-2–negative children. Isolated runny nose presented in 10.8% of SARS-CoV-2–negative versus 9.5% of SARS-CoV-2–positive children. All children with isolated diarrhea (n = 5), isolated headache (n = 3), and isolated rash (n = 2) tested negative. Preliminary symptom data based on 176 children from a second site showed that 9.9% of symptomatic children had a positive test result. Conclusions: Runny nose or nasal congestion was the most frequently reported symptom in all children tested for SARS-CoV-2. However, isolated runny nose or nasal congestion identified 2 cases of COVID-19 in our cohort. Eye redness or discharge may be an important symptom to screen for COVID-19 in children. Further research with a larger number of positive cases is needed to make conclusions about improving efficiency and efficacy of symptom screeners for COVID-19 in children.
Funding: No
Disclosures: None
Table 1. 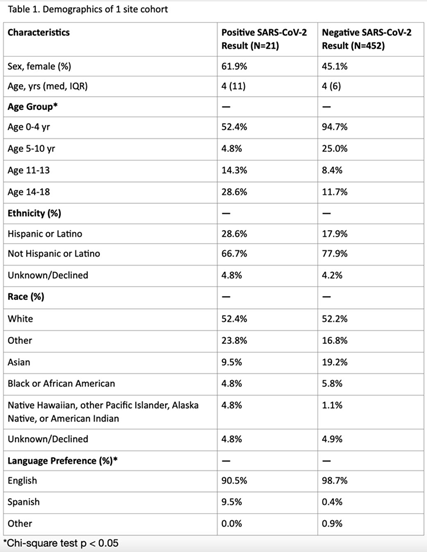
Table 2. 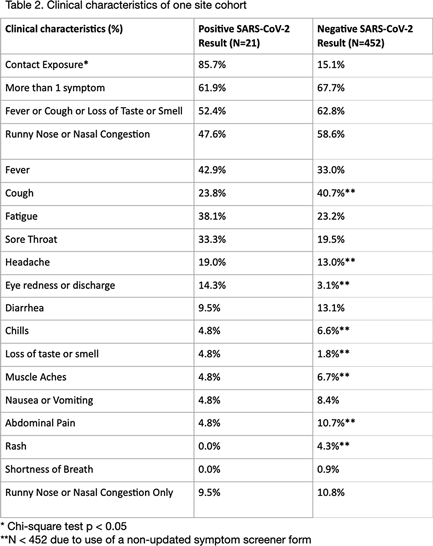
3259 Identifying the barriers and disparities for referral to kidney transplantation faced by HIV-infected patients with End Stage Renal Disease.
- Ruth Adekunle, Aneesh Mehta, Rachel Patzer, Wendy Armstrong, Ashley Burroughs
-
- Journal:
- Journal of Clinical and Translational Science / Volume 3 / Issue s1 / March 2019
- Published online by Cambridge University Press:
- 26 March 2019, p. 90
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/SPECIFIC AIMS: Our study aims to create a novel state level HIV-ESRD dataset and compare patient-level characteristics on rates of transplant referral, evaluation, waitlisting, and transplantation for HIV-positive versus HIV-negative patients. Our main hypothesis is that HIV-positive patients in Georgia are less likely to be referred to kidney transplant compared with HIV-negative patients. METHODS/STUDY POPULATION: Three datasets will be merged in order to create the HIV-ESRD dataset. The datasets are United States Renal Data System (USRDS), a southeast Transplant Referral Dataset and patient-level Georgia Department of Public Health HIV Incidence Database. The resulting study population will include patients that are older than 18, but less than 70, are HIV-positive and are on dialysis in Georgia. This dataset will also identify those patients who have been referred to transplantation, have been waitlisted, and have received kidney transplants between January 2012 and December 2017. If within a 1-year period, the prevalence of HIV-positive patients referred to transplant was lower than the 1-year period prevalence of HIV-negative patients for 3 consecutive years, the dialysis facility will be classified as having a within-facility disparity. We will then characterize patient level and dialysis facility-level factors that may contribute to observed findings. Patient characteristics will include demographic, clinical data, proxies of socioeconomic status, and geospatial relationships to transplant centers and rural vs urban neighborhoods. Facility-level characteristics includes profit status (profit vs. nonprofit), total number of staff (including full-time and part-time employees), aggregate demographic and clinical facility characteristics, and total number of treated patients. RESULTS/ANTICIPATED RESULTS:. We anticipate the successful creation of the proposed dataset that will allow for accurate identification of HIV-positive patients on dialysis in Georgia.. This dataset will provide the ability to determine referral, waitlisting, and transplantation rates.. We predict the overall rate of referral, waitlisting, and kidney transplantation in HIV patients will be relatively low, and that dialysis facilities with a higher proportion of HIV-positive will have lower referral rates compared to dialysis facilities treating a higher proportion of HIV-negative patients. It is foreseen that among patient-level characteristics, the strongest predictor for decreased referral rates will be HIV serostatus and among dialysis facility factors, profit status will be associated with decreased referral rates. DISCUSSION/SIGNIFICANCE OF IMPACT: This pilot study offers the creation of the first regional dataset of HIV-ESRD patients that will include patient-level characteristic of HIV-positive patients and provide a model for other states to adopt. We will contribute improved state-level description of incidence data of HIV-positive patients on dialysis, current rates of transplant referral, waitlisting, and transplantation, and offer potential associated factors that influence these processes. This knowledge will be used to determine the next steps in improving access to care; conducting qualitative research to understand dialysis facility views on transplant in HIV patients, understanding HIV patient’s position on transplantation, providing education on the value of kidney transplant referral, and expanding the approach of combining patient level HIV data to the southeast.





